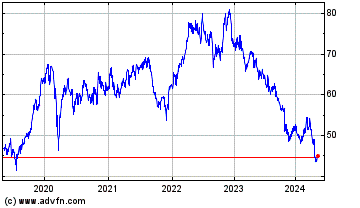
Bristol Myers Squibb (NYSE:BMY)
Historical Stock Chart
From May 2019 to May 2024
Full Commercialization Rights Transferred to Lilly
Eli
Lilly and Company (NYSE:LLY) and Bristol-Myers
Squibb Company (NYSE:BMY) today announced that the companies
have agreed to transfer rights to Erbitux® (cetuximab)
in North America, including the U.S., Canada, and Puerto Rico, from
Bristol-Myers Squibb to Lilly. Rights include, but are not limited to,
full commercialization and manufacturing operational responsibilities.
The companies’ decision comes after a 14-year successful collaboration,
which includes Lilly’s wholly-owned subsidiary ImClone LLC.
Bristol-Myers Squibb and Lilly will work closely to ensure a smooth
transition on this important product for patients with certain advanced
colorectal and head and neck cancers.
“Fully bringing Erbitux into the Lilly Oncology portfolio
accelerates Lilly’s commitment and leadership in gastrointestinal
cancers to include an effective treatment for advanced colorectal cancer
as well as head and neck cancer,” said Sue Mahony, Ph.D., senior vice
president and president of Lilly Oncology. “Our good work on Erbitux
began with its development at ImClone and has continued with
Bristol-Myers Squibb. We look forward to carrying on these efforts for
people battling select advanced colorectal and head and neck cancers.”
“Bristol-Myers Squibb is incredibly proud to have built Erbitux
into a major brand and an important therapy for so many patients with
certain colorectal and head and neck cancers,” said Murdo Gordon, head
of worldwide markets, Bristol-Myers Squibb. “This agreement further
aligns our Oncology organization with our prioritized opportunities in
immuno-oncology, across both solid tumors and hematologic malignancies.”
The transition is expected to be completed in the fourth quarter of
2015. Bristol-Myers Squibb will receive tiered royalties based on net
product sales in North America after the completion of the transition
through September 2018.
About Erbitux
Erbitux is an epidermal growth factor receptor (EGFR) antagonist
indicated for treatment of:
Head and Neck Cancer
-
Erbitux, in combination with radiation therapy, is indicated
for the initial treatment of locally or regionally advanced squamous
cell carcinoma of the head and neck (SCCHN)
-
Erbitux is indicated in combination with platinum-based therapy
with 5-FU for the first-line treatment of patients with recurrent
locoregional disease or metastatic squamous cell carcinoma of the head
and neck
-
Erbitux, as a single agent, is indicated for the treatment of
patients with recurrent or metastatic squamous cell carcinoma of the
head and neck for whom prior platinum-based therapy has failed
Colorectal Cancer
Erbitux is indicated for the treatment of KRAS
(wild-type), epidermal growth factor receptor (EGFR)-expressing,
metastatic colorectal cancer (mCRC) as determined by FDA-approved tests
for this use:
-
in combination with FOLFIRI (irinotecan, 5-fluorouracil, leucovorin)
for first-line treatment
-
in combination with irinotecan in patients who are refractory to
irinotecan-based chemotherapy
-
as a single agent in patients who have failed oxaliplatin- and
irinotecan-based chemotherapy or who are intolerant to irinotecan
Limitation of Use: Erbitux is not indicated for treatment of Ras-mutant
colorectal cancer or when the results of the Ras mutation
tests are unknown.
IMPORTANT SAFETY INFORMATION INCLUDING BOXED WARNINGS
Infusion Reactions
-
Grade 3/4 infusion reactions occurred in approximately 3% of
patients receiving ERBITUX® (cetuximab) in clinical trials, with fatal
outcome reported in less than 1 in 1000
-
Serious infusion reactions, requiring medical intervention and
immediate, permanent discontinuation of ERBITUX, included rapid
onset of airway obstruction (bronchospasm, stridor, hoarseness),
hypotension, shock, loss of consciousness, myocardial infarction,
and/or cardiac arrest
-
Immediately interrupt and permanently discontinue ERBITUX
infusion for serious infusion reactions
-
Approximately 90% of the severe infusion reactions were associated
with the first infusion of ERBITUX despite premedication with
antihistamines
-
Caution must be exercised with every ERBITUX infusion, as there
were patients who experienced their first severe infusion reaction
during later infusions
-
Monitor patients for 1 hour following ERBITUX infusions in a
setting with resuscitation equipment and other agents necessary to
treat anaphylaxis (eg, epinephrine, corticosteroids, intravenous
antihistamines, bronchodilators, and oxygen). Longer observation
periods may be required in patients who require treatment for
infusion reactions
Cardiopulmonary Arrest
-
Cardiopulmonary arrest and/or sudden death occurred in 4 (2%) of
208 patients with squamous cell carcinoma of the head and neck treated
with radiation therapy and ERBITUX, as compared to none of 212
patients treated with radiation therapy alone. In 3 patients
with prior history of coronary artery disease, death occurred 27, 32,
and 43 days after the last dose of ERBITUX. One patient with no prior
history of coronary artery disease died one day after the last dose of
ERBITUX. Fatal cardiac disorders and/or sudden death occurred in 7
(3%) of the 219 patients with squamous cell carcinoma of the head and
neck treated with platinum-based therapy with 5-fluorouracil (5-FU)
and European Union (EU)-approved cetuximab as compared to 4 (2%) of
the 215 patients treated with chemotherapy alone. Five of these
7 patients in the chemotherapy plus cetuximab arm received concomitant
cisplatin and 2 patients received concomitant carboplatin. All 4
patients in the chemotherapy-alone arm received cisplatin
-
Carefully consider the use of ERBITUX in combination with
radiation therapy or platinum-based therapy with 5-FU in head and
neck cancer patients with a history of coronary artery disease,
congestive heart failure, or arrhythmias in light of these risks
-
Closely monitor serum electrolytes, including serum magnesium,
potassium, and calcium during and after ERBITUX therapy
Pulmonary Toxicity
-
Interstitial lung disease (ILD), which was fatal in one case, occurred
in 4 of 1570 (<0.5%) patients receiving ERBITUX in Studies 1, 3, and
6, as well as other studies, in colorectal cancer and head and neck
cancer. Interrupt ERBITUX for acute onset or worsening of pulmonary
symptoms. Permanently discontinue ERBITUX for confirmed ILD
Dermatologic Toxicities
-
In clinical studies of ERBITUX, dermatologic toxicities, including
acneiform rash, skin drying and fissuring, paronychial inflammation,
infectious sequelae (eg, S. aureus sepsis, abscess formation,
cellulitis, blepharitis, conjunctivitis, keratitis/ulcerative
keratitis with decreased visual acuity, cheilitis), and
hypertrichosis, occurred in patients receiving ERBITUX therapy.
-
Acneiform rash occurred in 76-88% of 1373 patients receiving ERBITUX
in Studies 1, 3, 5, and 6. Severe acneiform rash occurred in 1-17% of
patients. Acneiform rash usually developed within the first 2 weeks of
therapy and resolved in a majority of the patients after cessation of
treatment, although in nearly half, the event continued beyond 28 days
-
Life-threatening and fatal bullous mucocutaneous disease with
blisters, erosions, and skin sloughing has also been observed in
patients treated with Erbitux. It could not be determined whether
these mucocutaneous adverse reactions were directly related to EGFR
inhibition or to idiosyncratic immune-related effects (eg, Stevens
Johnson syndrome or toxic epidermal necrolysis)
-
Monitor patients receiving ERBITUX for dermatologic toxicities and
infectious sequelae
-
Sun exposure may exacerbate these effects
ERBITUX Plus Radiation Therapy and Cisplatin
-
In a controlled study, 940 patients with locally advanced SCCHN were
randomized 1:1 to receive either ERBITUX in combination with radiation
therapy and cisplatin or radiation therapy and cisplatin alone. The
addition of ERBITUX resulted in an increase in the incidence of Grade
3-4 mucositis, radiation recall syndrome, acneiform rash, cardiac
events, and electrolyte disturbances compared to radiation and
cisplatin alone
-
Adverse reactions with fatal outcome were reported in 20 patients
(4.4%) in the ERBITUX combination arm and 14 patients (3.0%) in the
control arm
-
Nine patients in the ERBITUX arm (2.0%) experienced myocardial
ischemia compared to 4 patients (0.9%) in the control arm
-
The addition of ERBITUX to radiation and cisplatin did not improve
progression-free survival (the primary endpoint)
Electrolyte Depletion
-
Hypomagnesemia occurred in 55% of 365 patients receiving ERBITUX in
Study 5 and two other clinical trials in colorectal cancer and head
and neck cancer, respectively, and was severe (NCI CTC grades 3 & 4)
in 6-17%. In Study 2 the addition of EU-approved cetuximab to
cisplatin and 5-FU resulted in an increased incidence of
hypomagnesemia (14% vs 6%) and of grade 3–4 hypomagnesemia (7% vs 2%)
compared to cisplatin and 5-FU alone. In contrast, the incidences of
hypomagnesemia were similar for those who received cetuximab,
carboplatin, and 5-FU compared to carboplatin and 5-FU (4% vs 4%). No
patient experienced grade 3–4 hypomagnesemia in either arm in the
carboplatin subgroup. The onset of hypomagnesemia and accompanying
electrolyte abnormalities occurred days to months after initiation of
ERBITUX therapy
-
Monitor patients periodically for hypomagnesemia, hypocalcemia,
and hypokalemia, during, and for at least 8 weeks following the
completion of, ERBITUX therapy
-
Replete electrolytes as necessary
Increased Tumor Progression, Increased Mortality, or Lack of Benefit
in Patients with Ras-Mutant mCRC
-
Erbitux is not indicated for the treatment of patients with colorectal
cancer that harbor somatic mutations in exon 2 (codons 12 and 13),
exon 3 (codons 59 and 61), and exon 4 (codons 117 and 146) of either
K-Ras or N-Ras
-
Based on retrospective subset analyses of Ras-mutant and wild-type
populations across several randomized clinical trials of
anti-EGFR-directed monoclonal antibodies, including Study 4, use of
cetuximab in patients with Ras mutations resulted in no clinical
benefit with treatment related toxicity
Late Radiation Toxicities
-
The overall incidence of late radiation toxicities (any grade) was
higher with ERBITUX in combination with radiation therapy compared
with radiation therapy alone. The following sites were affected:
salivary glands (65% vs 56%), larynx (52% vs 36%), subcutaneous tissue
(49% vs 45%), mucous membranes (48% vs 39%), esophagus (44% vs 35%),
and skin (42% vs 33%) in the ERBITUX and radiation versus
radiation-alone arms, respectively
-
The incidence of grade 3 or 4 late radiation toxicities was
similar between the radiation therapy alone and the ERBITUX plus
radiation therapy arms
Pregnancy and Nursing
-
In women of childbearing potential and men, appropriate contraceptive
measures must be used during treatment with ERBITUX and for 6 months
following the last dose of ERBITUX. ERBITUX may be transmitted from
the mother to the developing fetus, and has the potential to cause
fetal harm when administered to pregnant women. ERBITUX should only be
used during pregnancy if the potential benefit justifies the potential
risk to the fetus
-
It is not known whether ERBITUX is secreted in human milk. IgG
antibodies, such as ERBITUX, can be excreted in human milk. Because of
the potential for serious adverse reactions in nursing infants from
ERBITUX, a decision should be made whether to discontinue nursing or
to discontinue ERBITUX, taking into account the importance of ERBITUX
to the mother. If nursing is interrupted, based on the mean half-life
of cetuximab, nursing should not be resumed earlier than 60 days
following the last dose of ERBITUX
Adverse Reactions
-
The most serious adverse reactions associated with ERBITUX are
infusion reactions, cardiopulmonary arrest, dermatologic toxicity and
radiation dermatitis, sepsis, renal failure, interstitial lung
disease, and pulmonary embolus
-
The most common adverse reactions associated with ERBITUX (incidence
≥25%) across all studies were cutaneous adverse reactions (including
rash, pruritus, and nail changes), headache, diarrhea, and infection
-
The most frequent adverse reactions seen in patients with carcinomas
of the head and neck receiving ERBITUX in combination with radiation
therapy (n=208) versus radiation alone (n=212) (incidence ≥50%) were
acneiform rash (87% vs 10%), radiation dermatitis (86% vs 90%), weight
loss (84% vs 72%), and asthenia (56% vs 49%). The most common grade
3/4 adverse reactions for ERBITUX in combination with radiation
therapy (≥10%) versus radiation alone included: radiation dermatitis
(23% vs 18%), acneiform rash (17% vs 1%), and weight loss (11% vs 7%)
-
The most frequent adverse reactions seen in patients with carcinomas
of the head and neck receiving EU-approved cetuximab in combination
with platinum-based therapy with 5-FU (CT) (n=219) versus CT alone
(n=215) (incidence ≥40%) were acneiform rash (70% vs 2%), nausea (54%
vs 47%), and infection (44% vs 27%). The most common grade 3/4 adverse
reactions for cetuximab in combination with CT (≥10%) versus CT alone
included: infection (11% vs 8%). Since U.S.-licensed ERBITUX provides
approximately 22% higher exposure relative to the EU-approved
cetuximab, the data provided above may underestimate the incidence and
severity of adverse reactions anticipated with ERBITUX for this
indication. However, the tolerability of the recommended dose is
supported by safety data from additional studies of ERBITUX
-
The most frequent adverse reactions seen in patients with KRAS
mutation-negative (wild-type), EGFR-expressing metastatic colorectal
cancer treated with EU-approved cetuximab + FOLFIRI (n=317) versus
FOLFIRI alone (n=350) (incidence ≥50%) were acne-like rash (86% vs
13%) and diarrhea (66% vs 60%). The most common grade 3/4 adverse
reactions (≥10%) included: neutropenia (31% vs 24%), acne-like rash
(18% vs <1%), and diarrhea (16% vs 10%). U.S.-licensed ERBITUX
provides approximately 22% higher exposure to cetuximab relative to
the EU-approved cetuximab. The data provided above are consistent in
incidence and severity of adverse reactions with those seen for
ERBITUX in this indication. The tolerability of the recommended dose
is supported by safety data from additional studies of ERBITUX
-
The most frequent adverse reactions seen in patients with KRAS
mutation-negative (wild-type), EGFR-expressing metastatic colorectal
cancer treated with ERBITUX + best supportive care (BSC) (n=118)
versus BSC alone (n=124) (incidence ≥50%) were rash/desquamation (95%
vs 21%), fatigue (91% vs 79%), nausea (64% vs 50%), dry skin (57% vs
15%), pain-other (59% vs 37%), and constipation (53% vs 38%). The most
common grade 3/4 adverse reactions (≥10%) included: fatigue (31% vs
29%), pain-other (18% vs 10%), rash/desquamation (16% vs 1%), dyspnea
(16% vs 13%), other-gastrointestinal (12% vs 5%), and infection
without neutropenia (11% vs 5%)
-
The most frequent adverse reactions seen in patients with
EGFR-expressing metastatic colorectal cancer (n=354) treated with
ERBITUX plus irinotecan in clinical trials (incidence ≥50%) were
acneiform rash (88%), asthenia/malaise (73%), diarrhea (72%), and
nausea (55%). The most common grade 3/4 adverse reactions (≥10%)
included: diarrhea (22%), leukopenia (17%), asthenia/malaise (16%),
and acneiform rash (14%)
Please read the U.S.
Full Prescribing Information including Boxed WARNINGS.
About Eli Lilly and Company
Lilly is a global healthcare leader that unites caring with discovery to
make life better for people around the world. We were founded more than
a century ago by a man committed to creating high-quality medicines that
meet real needs, and today we remain true to that mission in all our
work. Across the globe, Lilly employees work to discover and bring
life-changing medicines to those who need them, improve the
understanding and management of disease, and give back to communities
through philanthropy and volunteerism. To learn more about Lilly, please
visit us at www.lilly.com
and http://newsroom.lilly.com/social-channels.
About Bristol-Myers Squibb
Bristol-Myers Squibb is a global biopharmaceutical company whose mission
is to discover, develop and deliver innovative medicines that help
patients prevail over serious diseases. For more information, please
visit www.bms.com
or follow us on Twitter at http://twitter.com/bmsnews.
Erbitux is a trademark owned by or licensed to Eli Lilly and
Company, its subsidiaries, or affiliates.
Bristol-Myers Squibb and Eli Lilly and Company Forward-Looking
Statement
This press release contains "forward-looking statements" (as that
term is defined in the Private Securities Litigation Reform Act of 1995)
regarding the parties’ North American collaboration for ERBITUX. Such
forward-looking statements are based on current expectations and involve
inherent risks and uncertainties, including factors that could delay,
divert or change any of them, and could cause actual outcomes and
results to differ materially from current expectations. Among other
risks, there can be no guarantee that the transition will be completed
in the timeframe described in this release. In addition, the amount of
royalties paid to Bristol-Myers Squibb through September 2018 may differ
from current expectations. Forward-looking statements in this press
release should be evaluated together with the many uncertainties that
affect Bristol-Myers Squibb's and Lilly’s businesses, particularly those
identified in the cautionary statement and risk factors discussion in
Bristol-Myers Squibb's and Lilly’s Annual Reports on Form 10-K for the
year ended December 31, 2014, in their Quarterly Reports on Form 10-Q
and their Current Reports on Form 8-K. Neither Bristol-Myers Squibb nor
Lilly undertakes any obligation to publicly update any forward-looking
statement, whether as a result of new information, future events or
otherwise.
MediaBristol-Myers SquibbKen Dominski, 609-252-5251ken.dominski@bms.comorSarah
Koenig, 609-252-4145sarah.koenig@bms.comorEli
Lilly and CompanyCrystal Livers-Powers, 317-476-4160livers_powers_crystal@lilly.comorInvestorsBristol-Myers
SquibbRanya Dajani, 609-252-5330ranya.dajani@bms.comorEli
Lilly and CompanyPhil Johnson, 317-655-6874johnson_philip_l@lilly.com

